Sarcoidosis commonly presents with abnormalities identified incidentally on chest radiography. Systemic symptoms such as fever, night sweats, and weight loss are common. Sarcoidosis can affect the lungs, with symptoms such as chest pain, shortness of breath, cough, and most commonly, pronounced fatigue. It can also affect the peripheral lymph nodes, heart, kidneys, gastrointestinal tract, central nervous system (CNS), liver, spleen, bone, muscle, and endocrine glands. Venous thromboembolism and pulmonary hypertension are potential complications of sarcoidosis. Approximately 90% of patients will have lung involvement. Pulmonary fibrosis and bronchiectasis result in "honeycombing" of the lung and represent end-stage lung disease due to chronic granulomatous inflammation. Hilar lymphadenopathy is asymptomatic and affects 80% of patients. Approximately 3%-12% of patients have hypercalcemia.
Granulomas of the eyelids, lacrimal glands, conjunctiva, iris, retina, and choroid can occur. Rarely, there can be granulomatous inflammation of the extraocular muscles leading to diplopia, which may be the presenting sign of sarcoidosis.
Ten to thirty percent of patients will present with Löfgren syndrome with arthritis, erythema nodosum, and bilateral hilar adenopathy, although rates vary by population. Women more commonly have erythema nodosum, and men more commonly have ankle periarticular inflammation or arthritis.
Neurosarcoidosis commonly manifests as cranial-nerve deficits. Any part of the neurologic system can be impacted by sarcoidosis; a vast range of neurologic signs and symptoms may be present.
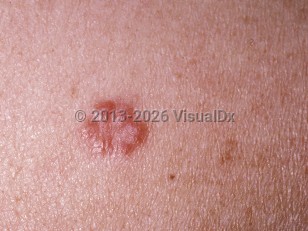
Cutaneous disease is often the first sign of systemic sarcoidosis. Approximately 25%-35% of patients will have cutaneous involvement, and some patients may have skin-limited disease. Asymptomatic red-brown dermal papules and/or plaques that favor the face, neck, upper extremities, and upper trunk are the most common specific cutaneous sarcoid lesions.
There are several other morphologic variants of cutaneous sarcoidosis. Lupus pernio, papular / plaque sarcoidosis, hypopigmented macules, ulcerative lesions, psoriasiform sarcoidosis, and scalp sarcoidosis occur more frequently in Black individuals than White individuals.
Some drugs and exposures have been associated with the development of sarcoidosis and sarcoid-like granulomatosis. Patients undergoing antiviral therapy for chronic hepatitis C – both monotherapy with IFN-alpha and combination therapy with IFN-alpha and ribavirin – have developed new-onset sarcoidosis or experienced reactivation of preexisting sarcoidosis during or shortly after treatment. The disease typically manifests as pulmonary and/or cutaneous sarcoidosis and follows a benign course, resolving spontaneously or within months after antiviral treatment is completed. More complicated multisystem cases, eg, involving the CNS, have been reported. In addition, there have been an increasing number of reports of new-onset sarcoidosis manifesting in patients who are receiving anti-tumor necrosis factor (TNF)-alpha therapy (etanercept, infliximab, adalimumab), eg, for a rheumatologic diagnosis. This is paradoxical because TNF-alpha inhibitors have been used to treat sarcoidosis. Cutaneous eruptions may occur in up to 50% of these patients, and pulmonary involvement may also be noted. The disease typically resolves with discontinuation of the drug and steroid therapy. It has been reported that exposure to moderate-to-high levels of silica increases the risk for sarcoidosis, which is of special concern for first responders (eg, firefighters). This association is more common in men due to occupational exposure.
Prognosis varies depending on a variety of factors. Those presenting with Löfgren syndrome, erythema nodosum, or stage I disease and those with initial improvement or spontaneous resolution of disease without therapy have a favorable prognosis, whereas those with more extensive lung involvement, extrapulmonary organ involvement, or multiorgan involvement, as well as those requiring treatment, Black individuals, and those of lower family income have a poorer prognosis.
Mortality associated with sarcoidosis is uncommon. It is generally due to significant granulomatous disease in the lungs and heart, leading to respiratory failure, cardiac arrhythmias, and heart failure. CNS, liver, and renal diseases are also causes of morbidity and mortality.
Pediatric patient considerations: Sarcoidosis is an uncommon disease in pediatric patients and is extremely rare in children younger than 6 years. When sarcoidosis presents in children younger than 6 years, it is characterized by a triad of skin rash, uveitis, and arthritis without intrathoracic involvement. In adolescents, the cutaneous manifestations of sarcoidosis are similar to those seen in adults, with the exception of lupus pernio and erythema nodosum, which are rare in that age group.



 Patient Information for
Patient Information for